
Eczema is a condition otherwise known as atopic dermatitis. Often found in children, it can affect people of all ages. While not life-threatening, it can make you wish you were dead depending on which part of the flare-up cycle you are experiencing.
More than 10 percent of the general United States population experiences some form of eczema. That’s between 15-25 percent of all dermatological patients. And most recent surveys show cases are on the rise.
Eczema is a chronic condition that comes and goes, and it thankfully can be managed if you know what you are dealing with and the best approach for action.
In the article to follow, we’ll go over the symptoms, causes, different types, treatments, therapies, and remedies. Let’s get down to it.
Eczema Symptoms
The condition of eczema is characterized by dry and itchy patches of skin. In more extreme cases, it can bring about blisters and pus, usually situated on a yellowish to light brown crust of skin.
While it sounds horrible when put like that — and it can be — many simply experience mild cases of it when they come into contact with an irritant of some sort. Other eczema-sufferers have problems that go deeper.
What are the main causes of eczema?
Lots of things can cause eczema, and it is important to know the culprit if you are going to take the appropriate treatment. While it can certainly run in the family, the more direct factors are as follows.
When Hormones Cause Eczema
Pregnancy and certain portions of the menstrual cycle are key times when a woman’s hormones are changing. Another time is around menopause. Eczema frequently follows one of these life events.
In fact, one study found that of 500 women experiencing skin conditions during their pregnancy, 50 percent were eczema cases.
Stress and Eczema
Doctors agree that stress is a trigger for eczema. As stress levels rise, symptoms often become more pronounced, so there is a dynamism that your feelings and emotions can bring to the condition.
With this in mind, it’s no wonder that children outnumber adults when it comes to experiencing the condition.
After all, when you are a child, you don’t have full command of your emotions, and you have not yet worked out how to deal with the simplest of stressors.
Your body and mind are more susceptible to reacting negatively to any change, and in that age range, the changes are coming fast and furious.
Foods Can Trigger
It is unfortunate, but some of the most delicious foods can only make your eczema worse, particularly when you are in a flare-up period.
Cow’s milk, eggs, soy products (yep, we actually like soy products), gluten, nuts, fish, and shellfish, are among the many no-no’s.
Track your calories by keeping your food journal so you can stay fit and have the awareness needed to avoid trouble items.
Microbes
There is significant evidence to suggest that bad eczema flare-ups in children are caused due to Staphylococcus aureus bacteria. The bacteria “is commonly found on skin,” Wong notes, adding that “its exact role in the condition is unclear.”
If one microbe can do this, why not another? Lesson being: there is enough of a bacterial connection to put this on the radar, but we’ve still got a lot to learn about the direct impact.
Allergens
Allergic contact dermatitis, another form of eczema, produces three million new cases per year in the U.S. alone. It is brought about by a common or uncommon allergen making contact with the skin.
Pollens, ragweed, and mold can all be responsible, but some of the others on this list can cross over into this category. Case in point…
Chemicals and Irritants
Smoke, soap, cosmetics, fragrances, jewelry, and poison ivy, are all chemicals and irritants that can light up your skin like a Christmas tree. Keep a careful watch on the things you’re wearing or working around.
If you avoid the trigger, your eczema can clear up in a couple of weeks.
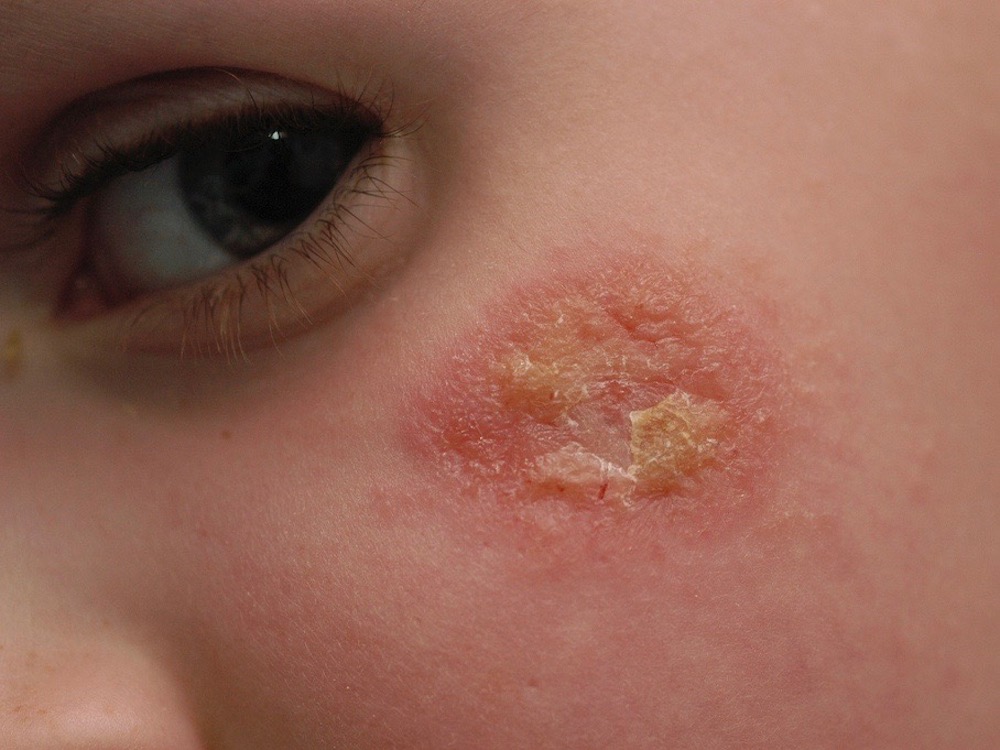
Eczema can form in dry, scaly patches on the face, and it is most common in children.
What skin conditions fall under the eczema family?
The word eczema is a catch-all for different types of skin conditions that bear similarities to one another while veering slightly off-path based on cause and area affected. To determine what you’re dealing with, first consult the list below.
Stasis dermatitis
Do your lower legs ever turn uncontrollably itchy during certain times of year? (Winter is our weak spot.) If so, you may be experiencing Stasis dermatitis.
According to the American Academy of Dermatology, Stasis dermatitis “is most common in the lower legs because leg veins have one-way valves, which play an important role in circulating our blood.
These valves push blood up the legs. As we age, these valves can weaken and stop working properly. Some blood can leak out and pool in the legs.” Dermatologists may refer to this as “venous (vee-nis) insufficiency,” the organization notes.
Seborrheic eczema
The condition of Seborrheic eczema is characterized by the development of red, scaly patches on the skin, particularly situated on the scalp.
According to the National Eczema Association, the condition also can appear on the chest, face, and upper back — pretty much anywhere that features a rich deposit of sebaceous (oil-producing) glands.
It is the main culprit when it comes to the development of dandruff, so if you’re thinking about getting rid of the problem by cutting off all your hair, don’t. It’s a glandular problem, not a follicle one.
Nummular eczema
Ever wonder why your arms and legs are developing those coin-shaped lesions that may feel sore or itchy? If you’re like millions of Americans, they probably panic you enough to hit the Internet and see which form of cancer it could possibly be.
Well, not all roads lead to cancer, so search responsibly and avoid worrying yourself to death. This particular scenario is a harmless albeit annoying development known as Nummular eczema, which, the AAD notes, can last for “weeks or months” before clearing up on their own.
Men are the most likely victims of this one, though it does hit female teenagers and young adults quite a bit, too.
Neurodermatitis
Neurodermatitis can be particularly worrisome because it is a condition that can progress rapidly the more you scratch it, and the more you scratch it, the more you will want to scratch it.
Signs and symptoms, the Mayo Clinic notes, include a single or multiple itchy skin patches of a leathery or scaly nature. They also can be raised, rough patches that are “red or darker than the rest of your skin.”
Incessant scratching can worsen the condition rapidly and become infected. If you notice a progression, consult with a medical professional.
Dyshidrotic eczema
Dyshidrotic eczema is one of the less common forms of eczema that can attack the fingers and palms of your hands. The condition is characterized by small fluid-filled blisters that develop on affected areas.
Science knows considerably less about this one than some of the others presented here, but they do believe physical/emotional stress and exposure to allergens can either create or exacerbate the condition, so addressing those issues could help alleviate the effects.
Allergic contact dermatitis
This one, we’ve already spoken about, but just to recap, things come into contact with your skin — be they naturally occurring (pollen, ragweed) or food- and chemically-based — and they create problems.
According to the American Academy of Allergy, Asthma, and Immunology (AAAAI), allergic skin conditions can take anywhere from 14 to 28 days to go away, and breakouts may occur within 48 hours of contact.
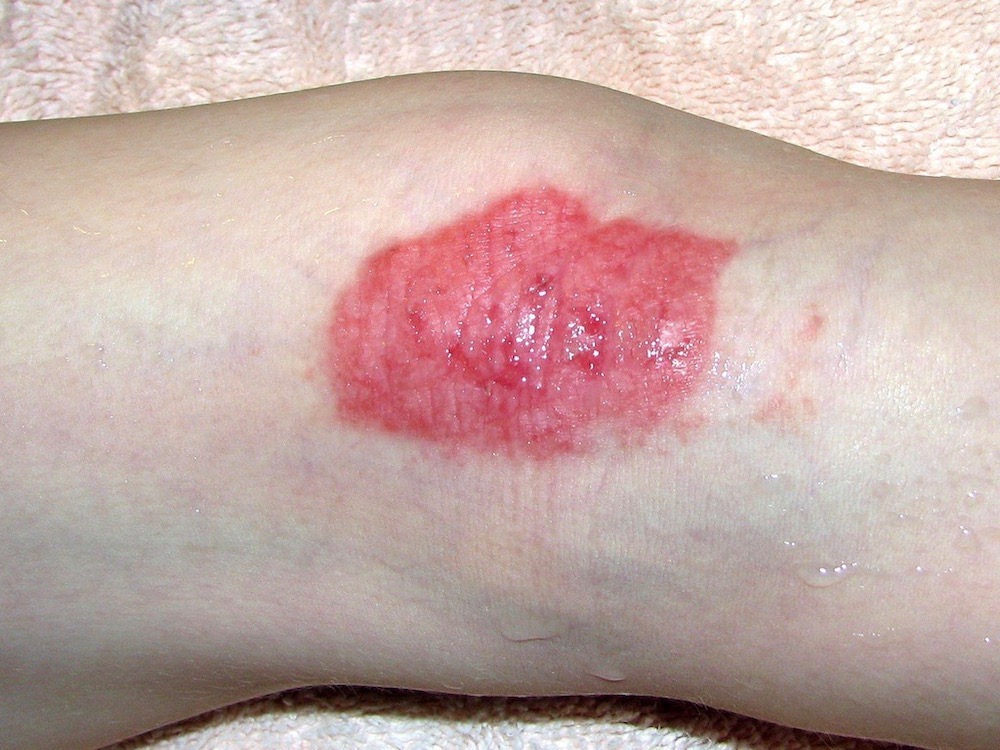
Allergic contact eczema is just one of the many forms of the skin condition. Shown here, the back of a patient’s knee.
Eczema can cause eye complications, too
Changes in appearance to your eyes may not be immediately connected to the condition of eczema, but they can certainly be related. In fact, let’s look at all the ways that eczema can affect your eyes, eyelids, and surrounding area.
Inflammation of the eyelids
Some cases of eye-related eczema involve inflammation of the eyelids, which can result in some pretty icky results. Examples, notes Stewart, are “itching, burning, watering of the eyes, and mucous discharge.”
“This can also cause a cobblestone pattern of skin to develop underneath the eyelids, which can interfere with wearing contact lenses,” she added.
Deformed corneas
Eyelid itching is inevitable when it comes to the development of eczema in that area, and whenever you give into it, you could be doing damage to your corneas from the trauma of hard rubbing and pressing and pulling (however you get relief).
Greater risk of cataracts
In an interview with Tanya Kormeili, MD, assistant clinical professor in the department of dermatology at the University of California at Los Angeles, Stewart also found that atopic cataracts can develop in patients with long-standing atopic disease of 10 or more years.
“The incidence of atopic cataracts is estimated at 10 percent, most often affecting both eyes,” she notes.
Retinal detachment
Eye-eczema sufferers experience retinal deatchment in greater numbers, and the condition can occur without much warning. When the retina detaches, you can have loss of peripheral vision or worse.
Retinal detachment is common with “inflammation, vascular abnormalities, or injury” that cause fluids to build up under the retina, so it’s no surprise why a condition like eczema might affect it between the condition’s behaviors and the trauma that you inflict upon the eye in an effort to get relief.
Spot-scarring throughout the eye
Thankfully, this one is rarer than some of the other conditions you’ll find on this list, but it is entirely possible eye scarring could occur.
When you experience eye scarring, you could end up with chronic haziness in your field of vision, and good luck ever enjoying a book or movie again at that point.
It is correctable, but the correction is rather unpleasant. The American Academy of Opthalmology explains that removal of scar tissue requires “vitrectomy membrane dissection surgery,” adding that “if there is scar tissue with a retinal detachment (when the light sensitive tissue peels away from the back of the eye) then a more involved vitrectomy surgery is needed.”
These surgeries are invasive and can often take several hours to perform.
What eczema treatments are there?
When you are looking into treatments for your eczema, you want to hone in on four key areas of concern. Whatever you do, you want it to be able to control the itching, repair the skin, and prevent flareups and infections.
There are a number of methods that doctors have used to do this, and we’re about to go into each one.
It is also worth noting, however, that you might be able to control the condition on your own without medical assistance. We’ll give you some tips for that, too. Let’s bring it home and start with…
Barrier repair moisturizers
Since eczema manifests as dry and itchy skin, it is possible to treat through the use of a moisturizer, though you will want to make sure said moisturizer lacks any chemicals or irritants that might make the problem worse.
Barrier repair moisturizers are available at a variety of price points. Verywell Health has an excellent rundown of the 6 Best Ceramide Creams for Eczema and Dry Skin right here.
Corticosteroids
These may come in the form of creams, solutions, foams, or ointments. Doctors often prescribe corticosteroids to help fight the effects of an eczema flare. But just what are corticosteroids, and how do they work?
Corticosteroids are produced in the adrenal cortex of vertebrates like you and me. They “mimic the effects of hormones your body produces naturally in your adrenal glands, which sit on top of your kidneys.
When prescribed in doses that exceed your body’s usual levels,” they reduce or suppress inflammation.
NSAID ointments
NSAID stands for “nonsteroidal anti-inflammatory drug,” and how they work is pretty self-explanatory from the long description. Medicines like Bayer, Bufferin, Excedrin, Advil, Motrin IB, and Aleve are NSAIDS.
For eczema, however, the preferred method of delivery is an ointment because you can place the NSAID directly on the affected area, thus shortening the amount of time that it takes for the drug to become effective.
Topricin and Aspercreme are two popular examples of NSAID ointments. These topicals also are useful when dealing with arthritis, according to the Arthritis Foundation.
Pimecrolimus, tacrolimus solutions
Pimecrolimus works by decreasing an eczema sufferer’s immune system, thus slowing the growth of eczema. Considering its manipulations on the immune system, it is generally used as a next resort drug when others have failed.
Tacrolimus essentially works the same. A very small number of users have developed cancers, but medical research hasn’t progressed far enough along to know whether these had anything to do with it. Just somethign to keep in mind.
Antibiotics
Antibiotics are frequently used to address eczema, particularly the kind that might have been caused by microbial infection. Antibiotics work by murdering bacteria one-by-one.
The downside — learned the hard way — is that it can wipe out good bacteria, too, thus causing digestive problems.
They’re also worthless when it comes to viral infections. (Those have to run their course.)
When you don’t have healthy bacteria in your system, as in good gut bacteria, you can experience digestive issues as a result of taking antibiotics. Not to fear.
Just use probiotics to replenish, and that will likely do the trick. As in all things, however, talk to your doctor first.
Antihistamines
A histamine is a compound that cells release in response to injury and in allergic and inflammatory reactions. The release causes contraction of smooth muscle and dilation of capillaries.
Histamines definitely have their purpose, but when they go rogue, it can cause significant inflammation and itching.
An antihistamine counteracts these effects, so it’s always good to have some on-hand during allergy seasons and whenever you experience an inflammation of any kind. (Hello, eczema.)
Allegra and Benadryl are two of the most popular antihistamine brand names.
Phototherapy
Eczema varies in severity from one person to the next, so if none of the above options are doing it for you, you might consider this outside-the-box method. In fact, it is a “second-line option” for when topical drugs have failed.
Also known as UV light therapy, it appears to reduce the number of white cells (T-cells) in the skin, which are responsible for causing inflammation and are known to play an important part in the development of eczema, the site notes.
As a result, your skin becomes red, itchy, and sore. “Improvement with phototherapy happens gradually after several weeks of regular treatments. There is a reduction of itching and the eczema slowly clears as treatments continue.
Once there is absence of itching and clearance of most, if not all, of the active eczema, a controlled period of reducing the frequency of treatments is often used successfully to ‘wean the patient off,’ thereby reducing any likelihood of (recurrence),” the site adds.
The drawback: this is something you generally have to do at a clinic in order to be effective, and that will cost you.

A warm bath may not be able to cure your eczema, but it can cut down on the effects and make life a little easier.
Home Remedies for Eczema
With all the costlier remedies accounted for, let’s close by discussing some ways that you can alleviate pain and discomfort and maybe even fend off an eczema attack, all without spending a lot of money.
Take warm baths
Warm water will knock out some of the inflammation and keep the eczema clean, thus reducing the likelihood of infection. Plus, who doesn’t feel great after a nice, warm bath?
And this is one activity where you can enjoy a glass of wine while you’re doing it.
Use daily moisturizers
Skin hydration is important to keeping the eczema-causing inflammation down; again, just make sure that there isn’t an irritant in the moisturizer itself.
Cut back on the showers and hand-washing
While a warm bath can help, daily showers and scrubbing with harsh soaps can cause continuous damage to the skin that creates an hospitable environment for eczema to return.
If you absolutely must shower every day, try to keep all-over washing to every other day. On the “off days,” hit the areas that are most likely to be problematic from a sweat/stench perspective (feet, armpits, and genital regions).
While not showering every day may seem gross to you, keep in mind that oil production goes down as you get older. If you’re coming at this during your refinery stages (the teen years and young adult), then not showering every day is kinda gross.
But if your body has stopped producing so much glandular stuff, you’ll be fine skipping days, and no one will be the wiser.
Wear cotton and choose the right fit
Fabrics — whether in texture, tightness, or both — can serve as irritants to your skin, and that irritation might contribute to outbreaks.
Avoid getting overheated
Eczema thrives on heat and inflammation, so keeping the skin cool or comfortable will help it not to propagate, even if it doesn’t get rid of the problem altogether. This is more for managing the condition.
Know your triggers.
Eczema sufferers may have the condition in common, but they don’t necessarily have the causes in common. The more you know about what is triggering your condition, the better you will be at a) treating it, and b) reducing its effects.
Ease stress.
Cut out emotional toxicity, be it people or situations, as much as you possibly can.
In closing
When eczema first strikes and you’re not sure what you’re dealing with, it can cause apprehension. But the more you know about what causes it, what treatment options are at your disposal, and what you can do to manage the condition, the easier it will be to reclaim control of your life.
Want More Home Remedies You Can Use Around Your Home?
 Then get yourself a copy of the Home Remedies Toolkit downloadable guide with 215+ DIY recipes for making your own natural health and beauty products and non-toxic cleaning supplies. Each recipe is beautifully presented with stunning photography and will save you a fortune as you discover how to stop buying toxic products for your home, health and beauty regime and instead replace with better, greener and cheaper alternatives. Get your copy here.
Then get yourself a copy of the Home Remedies Toolkit downloadable guide with 215+ DIY recipes for making your own natural health and beauty products and non-toxic cleaning supplies. Each recipe is beautifully presented with stunning photography and will save you a fortune as you discover how to stop buying toxic products for your home, health and beauty regime and instead replace with better, greener and cheaper alternatives. Get your copy here.
Share Image on Pinterest







Leave a Reply